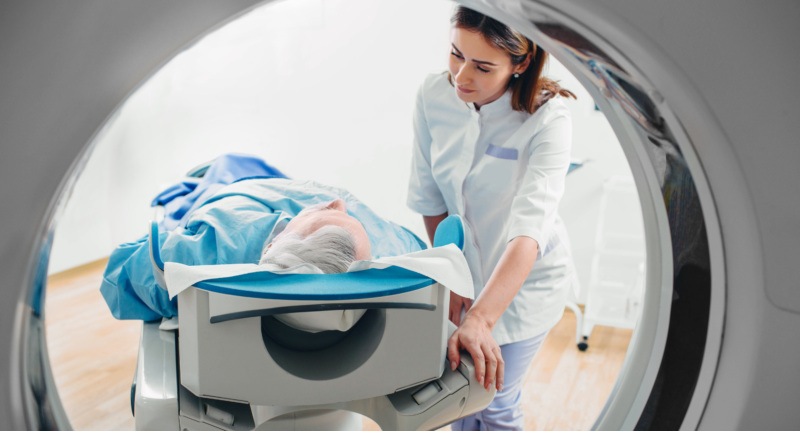
Ages 50–80: Low-dose CT scan
People who smoke cigarettes or used to smoke cigarettes may qualify for screening with a low-dose CT scan, an easy and painless screening procedure. Screening is recommended for those who have 20 pack-year histories of smoking.